Recent History
January 1, 1910
Über den Gehalt normaler und atheromatöser Aorten an Cholesterin und Cholesterinestern.
German chemist Adolf Otto Reinhold Windaus discovered atheromatous arterial lesions (arterial plaques) contain six times as much free cholesterol and 20 times as much esterified cholesterol as do healthy arteries
In 1910, as part of his pioneering studies of the role of cholesterol in human metabolism, German chemist Adolf Otto Reinhold Windaus discovered atheromatous arterial lesions (arterial plaques) contain six times as much free cholesterol and 20 times as much esterified cholesterol as do healthy arteries (2). Windaus would also later describe the pathways by which cholesterol is converted to vitamin D. For his work, he was awarded the Nobel Prize in chemistry in 1928.
The assumption at the time was, predictably, that the cholesterol in arterial plaques must arise from the cholesterol circulating in the bloodstream. In time, this finding gave rise to Gofman/Keys’ lipid hypothesis, which holds that elevated blood cholesterol concentrations (caused by eating a high-fat diet especially rich in “artery-clogging” saturated fats) drive cholesterol across the arterial lining, a single layer of cells known as the endothelium, and into the subendothelial space, causing the initiation of fatty streaks (Figure 1). These then progress to the development of more advanced atherosclerosis, termed arterial plaques (Figure 2), which among other complications can cause heart attacks and strokes.
Figure 1: This diagram explains the currently accepted theory of how endothelial damage, largely of unknown cause, allows LDL-cholesterol to cross the endothelium and enter a postulated and hypothetical acellular space, the subendothelial space. There, the LDL-cholesterol is taken up by macrophages, causing the development of the earliest form of atherosclerosis, known as the fatty streak. Note that for the atherosclerotic process to happen in this way, the tunica intima must be devoid of all cells other than the single layer of endothelial cells that coat its upper surface, separating it from the blood contained in the lumen of the artery. According to this model, the subendothelial space is essentially a wide-open vacant space waiting expectantly to accommodate these (complex) processes that produce atherosclerosis. Reproduced with additions from reference 4, p. 3.
The finer details in Figure 1 are not critical to the argument. What is important is the way in which the different cellular structures are depicted.
Here, the crucial point is that, according to the currently popular explanation of atherosclerosis (4), until the endothelium is damaged (by currently unknown biological events), allowing the unrestrained entry of LDL-cholesterol, the tunica intima is depicted as a single, thin layer of endothelial cells sitting on top of an acellular space (devoid of cells). This is an important consideration, since the presence of any cells in the subendothelial space must impede the entry of LDL-cholesterol directly from the bloodstream and will hinder the ability of the macrophages to detect and consume the cholesterol, as depicted in Figure 1.
Figure 2 depicts how this model explains the progression of the fatty streak to full-blown atherosclerotic plaque. Note again that the subendothelial space is devoid of cells before the hypothetical endothelial damage allows the free entry of LDL-cholesterol into this conveniently located anatomical space.
Figure 2: This figure shows how the fatty streak (Figure 1) progresses to the atherosclerotic plaque according to the lipid hypothesis. For the lipid hypothesis to be true, until after the initial “injury” to the endothelium has allowed the entrance of blood-derived LDL-cholesterol, the tunica intima must, as shown in this figure and in Figure 1, contain no cells other than the thin layer of endothelial cells on its upper surface. Notice that in this figure, smooth muscle cells (SMC) migrate from the tunica media into the tunica intima to further progress the development of the atherosclerotic plaque. Reproduced with additions from reference 4, p. 8.
In 1910, neither Windaus nor anyone else was aware that cholesterol cannot simply pass through healthy arterial walls, however hard it may be “shoved” (3). Currently, the most popular theory for atherosclerosis is that shown in Figures 1 and 2. This theory holds that the endothelial cells lining the lumen of the artery wall must first be damaged before the passing of cholesterol through the wall can happen. This is termed “endothelial cell dysfunction” (4), but the immediate cause of “endothelial cell dysfunction,” if this is indeed the mechanism, remains shrouded in secrecy even today, 110 years after Windaus’ discovery.
This theory also predicts that cholesterol enters damaged arteries down a concentration gradient, so the degree of a person’s arterial disease can be predicted quite simply as their average blood cholesterol concentration multiplied by the number of years the blood cholesterol concentration has been “elevated” (3, 5).
Also, still unknown then was that atherosclerosis is a patchy disease that selectively targets only specific areas of different arteries. This is exemplified by what happens in the coronary arteries supplying blood to the heart muscle (6).
It also was then unknown that in some populations, there may be advanced atherosclerosis in the cerebral (brain) arteries with minimal involvement of the coronary (heart) arteries (7, 8). In such cases, a person is at greater risk of stroke than heart attack. In other cases, as is more prevalent in the U.S., the opposite applies.
January 1, 1913
Anitschkow reported that he could induce atherosclerotic-type lesions in rabbits by feeding them huge amounts of cholesterol.
"Early evidence suggestively linking cholesterol to heart disease also came from animals. In 1913, the Russian pathologist Nikolaj Anitschkow reported that he could induce atherosclerotic-type lesions in rabbits by feeding them huge amounts of cholesterol. This experiment became quite famous and was widely replicated on all sorts of animals, including cats, sheep, cattle, and horses, leading to the widespread view that cholesterol in the diet--such as one finds in eggs, red meat, and shellfish--must cause atherosclerosis. Contemporaries noted that rabbits, along with most of the animals used in follow-up experiments, are all herbivores. They therefore do not normally eat animal foods and are not biologically designed to metabolize them. By contrast, when the experiment was replicated on dogs (which eat meat as humans do), the animals demonstrated an ability to regulate and excrete extra cholesterol."
Nina Teicholz - The Big Fat Surprise - Page 22
June 24, 1916
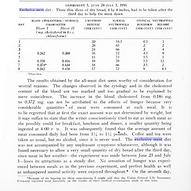
Studies on Cholesterol
The exclusive meat diet was not accompanied by any unpleasant symptoms whatsoever. No sensation of hunger was experienced between meals as in the previous experiment, and perfect health as well as unhampered mental activity were enjoyed throughout.
The slight initial increase observed in the blood cholesterol may have been due to the rather severe nature of the diet to which the body had to become accustomed. On the first day the writer was chronically hungry and had a severe headache in consequence, but during the two following days she felt perfectly well and comfortable. It is a well-known fact that fasting is always accompanied by an increase of the blood cholesterol (Rothschild).** ‘The changes found in the cytology of the blood were still very slight, but the drop of the blood cholesterol to 0.186 mg. and the accompanying increase of lymphocytes and decrease of neutrophils is interesting when compared with the results of the subsequent experiments. The results obtained by the all-meat diet seem worthy of consideration for several reasons. The changes observed in the cytology and in the cholesterol content of the blood are too marked and too gradual to be explained by mere coincidence. The increase in the blood cholesterol from 0.186 mg. to 0.372 mg. can not be attributed to the effects of hunger because very considerable quantities of meat were consumed at each meal.
It is to be regretted that at first the exact amount was not determined by weight, but it may suffice to state that the writer conscientiously tried to eat as much meat as she possibly could for breakfast, luncheon and dinner, a smaller quantity being ingested at 4:00 p.m. It was subsequently found that the average amount of meat consumed daily had been from 1.25 to 1.5 pounds. Coffee and tea were taken as usual, but no alcohol, since it is never used. The exclusive meat diet was not accompanied by any unpleasant symptoms whatsoever, although it was found necessary to allow a very small quantity of dry bread after the third day, since meat in hot weather—the experiment was made between June 23 and July 1—loses its attractions as a steady diet. No sensation of hunger was experienced between meals as in the previous experiment, and perfect health as well as unhampered mental activity were enjoyed throughout.*.
On the seventh day, at the beginning of which the highest cholesterol value was registered, there was a slight attack of diarrhea. On the following day peristalsis was normal again, but the blood cholesterol had dropped to 0.342 per cent of cholesterol by the feces is one of the means by which the cholesterol balance is preserved (McNee), it seems logical increased peristalsis in order to maintain its equilibrium of health. regulation of the cholesterol balance was observed also more fully Since the elimination » assume that the body resorted to The fact that the same automatic regulation of the cholesterol balance was observed also in a later experiment would seem to support this view, and will be discussed in connection with Experiment 7. The gradual but steady drop in the lymphoid defense from 33 to 17 percent, the parallel increase of the polymorphoneutrophils from 46 to 72 per cent, and the unusual number of atypical neutrophils—9 percent ringforms, 12 per cent bizarre--which appeared in the blood as the cholesterol percentage reached its highest values, suggest a very definite relation between the chemical composition and the cytology of the blood, while the changes observed in both appear to be closely associated with the chemical nature closely associated the food consumed. The same observations could be made in every one of my experiments.
The cytologic changes found in the blood during the exclusive meat diet are moreover in perfect accordance with Gruner’s findings, which they corroborate. The two points on which he lays particular stress regarding the similarity between excessive meat consumption and in carcinoma the blood picture during atypical neutrophils inbetween reduction of the lymphocytes and the appearance of markedly increased numbers—seem to be borne out also by the following observations _______
The results obtained by the vegetable and fruit diet present a contrast as well as a complement to those of the exclusive meat diet. Whereas the blood cholesterol slowly but steadily decreased from 0.342 mg. to 0.202 mg. on the fifth day and finally seemed to settle down to a new standard, 0.242 mg., which was found on three consecutive days, the lymphoid defense increased from 17 per cent to 33 per cent, with a parallel drop in the neutrophils and a marked reduction of the number of atypical cells. In order to give the body sufficient time to swing back to normal values, and because of the tendency to collapse shown by the cubital veins, described above, eleven days were allowed to elapse before another blood test was made. During this interval the usual mixed diet was used again. The following values were found at its close: _______
Apart from the very slight increase in the neutrophil count, the normal stand ard had been reached again. ‘The difference between the original cholesterol standard, 0.272 mg., and the last reading, 0.266 mg., i. e., 0.006 mg., can hardly be considered significant. The intimate relation between the chemistry and the cytology of the blood and the diet, previously observed, seems to be confirmed by this experiment.
January 1, 1924
The American Heart Association is formed.
American Heart Association is Founded: Six cardiologists form the American Heart Association as a professional society for doctors. One of the founders, Dr. Paul Dudley White, described the early years as a time of “almost unbelievable ignorance” about heart disease.
January 1, 1937
Columbia University biochemists David Rittenberg & Rudolph Schoenheimer demonstrate that dietary cholesterol has very little effect on blood cholesterol.
"One of the early ideas for how people might lower cholesterol was simply to consume less of it. The notion that cholesterol in the diet would translate directly into higher cholesterol in the blood just seemed intuitively reasonable, and was introduced by two biochemists from Columba University in 1937. The assumption was that if we could avoid eating egg yolks and the like, we could prevent cholesterol from accumulating in the body."
-Nina Teicholz - The Big Fat Surprise - Page 23